+1 (951) 297 8375
Fax: +1 (951) 602
8264
contact@karmadocs.com
Mon - Fri: 9:00 AM - 5:00 PM
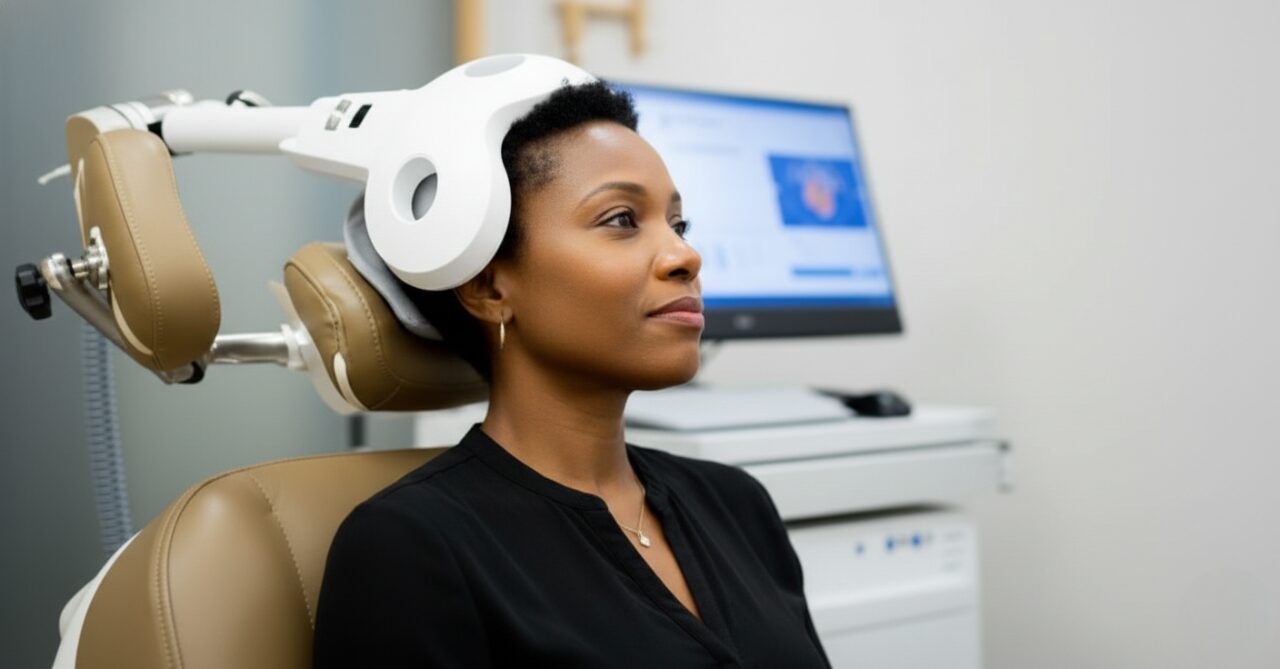
Transcranial Magnetic Stimulation (TMS) therapy has become an important treatment option for people who have not found enough relief from traditional approaches for depression and related mental health conditions. While many patients notice gradual improvement over time, some experience a temporary phase where symptoms seem to worsen. This often leads to concern and confusion, with many people asking is TMS dip normal and whether it is safe to continue treatment.
Related reading: learn about treatment-resistant depression and explore how TMS therapy can be covered by insurance.
According to Wikipedia’s article on major depressive disorder, MDD is a mood disorder that causes persistent feelings of sadness and loss of interest — and is one of the most studied and treatable mental health conditions in the world.
For individuals undergoing TMS Therapy in Palm Springs, understanding this phase is especially important so they do not feel discouraged or alarmed. A TMS dip can be unsettling, but in most cases, it is a short-term response as the brain adjusts to stimulation.
This guide explains what a TMS dip is, why it happens, how long it lasts, and how to cope with it—using clear and simple language.
A TMS dip refers to a temporary increase in depressive or emotional symptoms that some patients experience during the course of TMS treatment. Instead of feeling steady improvement, individuals may notice a drop in mood, increased anxiety, or emotional heaviness for a short period.
This dip does not mean the therapy has stopped working. Rather, it often occurs when the brain begins making bigger neurological changes. During this time, emotional regulation systems are being stimulated and reorganized, which can temporarily intensify feelings before stabilization occurs.
Yes, a TMS dip is normal for some patients, although not everyone experiences it. Many clinicians consider it a known response pattern during neuromodulation therapies like TMS.
Mental health recovery does not always follow a straight upward path. Just as physical rehabilitation can involve soreness before strength improves, the brain may go through a brief adjustment phase. Experiencing a dip does not mean the treatment is harmful or ineffective. In many cases, it signals that the brain is actively responding to stimulation.
Patients often wonder when does TMS dip happen, especially if they feel worse after initially feeling stable or hopeful.
Most people who experience a dip notice it:
This timing coincides with the phase when TMS begins altering communication between mood-related brain regions. Because these changes are internal and gradual, emotional responses may fluctuate temporarily.
TMS works by stimulating areas of the brain involved in mood, motivation, and emotional control—regions that may have been underactive for years due to depression.
As these areas become active:
This process can briefly overwhelm the nervous system, leading to mood fluctuations. The dip is often a sign that long-standing emotional suppression is lifting, which can feel uncomfortable before balance is restored.
TMS dip symptoms can vary in intensity and presentation, depending on the individual.
Commonly reported symptoms include:
These symptoms can feel intense but are usually short-term and reversible.
One of the biggest concerns patients have is how long does TMS dip last.
For most individuals:
The duration depends on individual brain chemistry, severity of symptoms, and overall stress levels. Importantly, the dip does not continue indefinitely and typically resolves without long-term effects.
No, not everyone experiences a dip. Many patients move through treatment with steady improvement or only mild emotional changes.
Factors that may influence whether a dip occurs include:
Each brain responds differently to stimulation, which is why experiences vary.
If you notice a dip during treatment, there are several supportive steps you can take.
One of the most important things to do during a TMS dip is to continue attending your scheduled sessions. Many patients feel tempted to stop treatment when symptoms worsen, but stopping early can interrupt the brain’s adjustment process. TMS works gradually, and the dip often occurs just before noticeable improvement begins.
Always inform your care team as soon as you notice changes in mood, anxiety, or energy levels. Open communication allows providers to closely monitor your response and make adjustments if needed. These may include changes in stimulation intensity, session timing, or supportive strategies to help you cope.
During a TMS dip, emotional resilience may be lower than usual. Tasks that once felt manageable—work responsibilities, social interactions, or problem-solving—can suddenly feel overwhelming. This does not mean you are regressing; it means your brain is underactive adjustment.
Try to reduce pressure wherever possible. Postpone non-urgent decisions, limit stressful conversations, and avoid overcommitting yourself. Giving your mind space to rest allows the nervous system to stabilize and makes it easier to move through this phase.
Sleep plays a crucial role in brain healing and emotional regulation. During a TMS dip, disrupted sleep can intensify symptoms such as low mood, irritability, and anxiety. Try to maintain a consistent sleep routine, go to bed at the same time each night, and limit screen exposure before sleep.
Physical rest is equally important. Feeling tired during a dip is common, as the brain is actively adjusting. Short naps, gentle movement, and avoiding overexertion can support recovery and help stabilize mood.
During a TMS dip, appetite changes are common. Some people eat less due to low motivation, while others may rely on irregular meals. However, poor nutrition and dehydration can worsen emotional instability and fatigue.
Try to maintain simple, regular meals even if your appetite is low. Focus on hydration and easily digestible foods. Stable nutrition helps support brain chemistry and prevents physical symptoms from worsening emotional distress.
For most people, a TMS dip is not dangerous and does not cause lasting harm.
However, if symptoms include:
Immediate communication with the treatment provider is essential. These situations are manageable with proper clinical support.
Many patients report that once the dip resolves, they experience:
This phase is often when patients begin to notice the true benefits of treatment.
So, is TMS dip normal? For many patients, the answer is yes. A temporary dip during treatment does not mean that TMS is failing or causing harm. Instead, it often reflects the brain’s process of adjusting, reorganizing, and responding to stimulation. Emotional healing is rarely linear, and short-term fluctuations can occur before meaningful improvement begins.
With proper guidance, open communication, and patience, most people can safely move through this phase and continue toward recovery. Patients supported by experienced teams, such as those at Karma Doctors & Associates, are often reassured when they understand that a TMS dip is temporary and manageable. Staying informed, supported, and consistent with treatment allows many individuals to experience the long-term benefits that TMS therapy is designed to provide.
A TMS dip is a temporary worsening of symptoms such as low mood, anxiety, or fatigue during the course of Transcranial Magnetic Stimulation (TMS) therapy. It typically occurs as the brain adjusts to new neural activity and rewiring.
Yes, a TMS dip is considered normal for many patients. It is a known response during treatment and does not indicate that the therapy is failing. In fact, it may signal that the brain is actively responding to stimulation.
A TMS dip most commonly occurs between weeks 2 to 4 or after multiple sessions, when deeper brain changes begin to take place.
For most patients, a TMS dip lasts a few days to up to two weeks. Symptoms typically improve as treatment continues and the brain stabilizes.
No, not everyone experiences a dip. Some patients improve steadily without any noticeable worsening of symptoms, while others may experience only mild fluctuations.